WHAT IS ULCERATIVE COLITIS?
Ulcerative colitis (UC) is a chronic, autoimmune disease that causes great inflammation of the colon, or large intestine. Ulcerative colitis is a form of Inflammatory Bowel Disease (IBD), with the other form being Crohn’s Disease. The primary difference between ulcerative colitis and Crohn’s disease is that the inflammation caused by ulcerative colitis specifically targets the colon, whereas the Crohn’s disease can cause inflammation in both the large and small intestine (entire gastrointestinal tract). Another fundamental difference between the two forms of IBD is that ulcerative colitis presents continuous inflammation, whereas with Crohn’s disease, it is more common to see healthy and inflamed tissue adjacent to each other (Kobayashi, T. et al). There are many possible culprits for the origination of ulcerative colitis. According to the Crohn’s and Colitis Foundation, some of these potential causes include abnormal immune responses to a virus or bacterial infection, environmental factors, or even genetics.
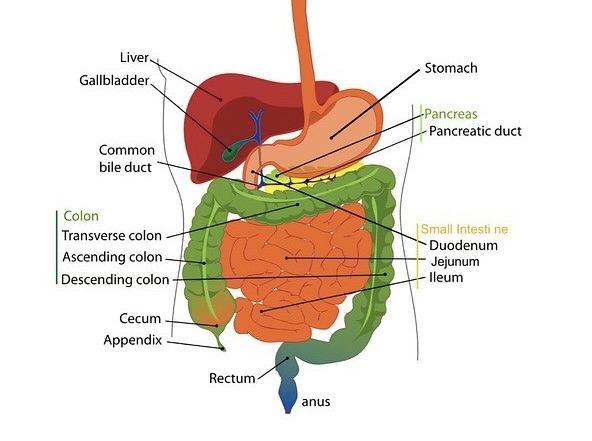
Diagram of Digestive/Gastrointestinal Tract